The return on investment from outsourcing data abstraction can be evaluated in two main ways —Financial ROI and Strategic ROI. How much weight and consideration each type of ROI gets will depend on your organization’s goals and current data abstraction staffing situation (or crisis).
From a Financial ROI perspective, outsourcing data abstraction can make an immediate quantifiable impact on your hospital’s budget and is usually most applicable in scenarios that involve abstractor turnover. With an existing or upcoming vacancy, a financial ROI analysis can inform whether your organization should keep that role in-house or offload the abstraction burden to a trusted outsourcing partner.
Strategic ROI, on the other hand, can often be a much stronger and more impactful reason to outsource. Many leading healthcare organizations, such as those on High Reliability journeys, are striving to elevate their position in the Hierarchy of Data Maturity (more on that later) by reinventing their approach to data. In short, this involves progressing beyond an army of passive data collectors and mobilizing/refocusing personnel to become active change agents.
In this whitepaper, we’ll detail how ADN clients have experienced the value of outsourcing data abstraction to a trusted partner so they can make more intelligent use of their financial and personnel resources, an emerging concept known as “Smartsourcing.”
Financial ROI
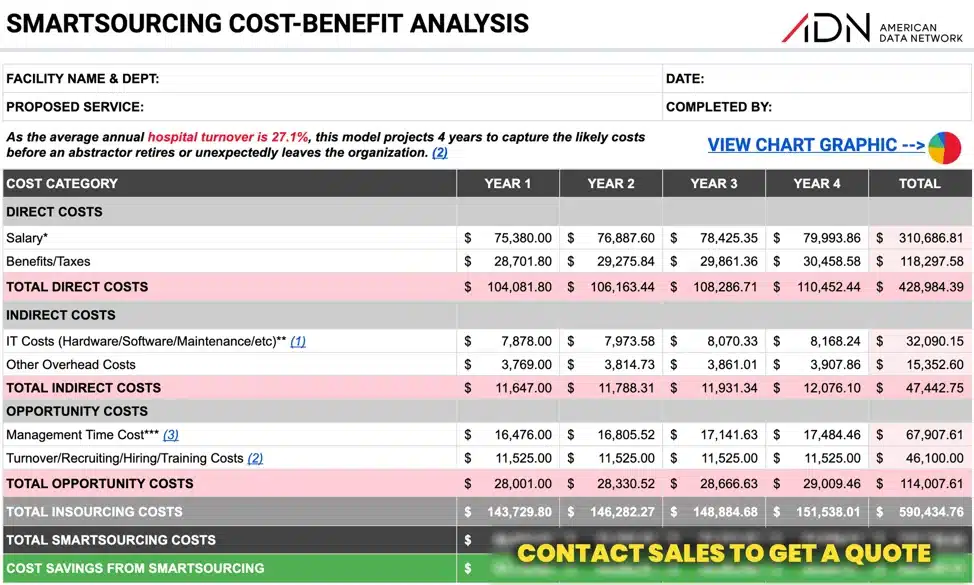
While calculating the Financial ROI — the predictable, tangible dollar value — is easier than the Strategic ROI, there are several considerations that are often overlooked. Calculating the blended salary, which includes benefits and taxes, as opposed to just the employee salary is a best practice. But beyond that, there are still quantifiable costs that can be eliminated from smartsourcing.
Let’s take a look at an average scenario to analyze the direct and indirect costs associated with an in-house abstractor. Labor market costs in Georgia are the median nationally, so we’ll use that for our example.
Direct Costs
The average salary for an RN in Georgia is $75,380. But the cost analysis doesn’t stop there. Using ADN’s Cost-Benefit Analysis Template, one can see that the salary only accounts for 54.8% of the total cost of an FTE. Benefits and taxes account for another $28,702. If only considering Salary and Benefits/Taxes in an abstractor compensation package, benefits/taxes account for between 27.6% – 31.0% depending on the state. When all tallied up, a salary of $75,380 actually has total direct costs to a hospital of $104,082.
Indirect Costs
IT and Overhead Costs
While perhaps less obvious, the indirect costs should not be overlooked or discounted. For example, in-house employees have an average of $7,878 in IT Costs (computer equipment and associated software expenses), according to the 2022 IT Spending & Staffing Benchmarks Report by Computer Economics. Other indirect costs related to overhead should also be factored in. Keeping a data abstractor’s knowledge base up to date often includes ongoing education like virtual or in-person conferences. Maintaining licenses and certifications also have associated expenses. Office space, furnishings and supplies are also a necessary cost of supporting an in-house employee. However, there isn’t definitive data to support an average for standard overhead. So ADN’s Cost-Benefit Analysis includes an optional line in which you can enter an estimate appropriate for your facility. (Your finance department should be able to provide a figure based on total overhead costs divided by the number of employees.)
Unknown Costs
There are also unknown costs associated with an in-house employee. While it is best factored into the Cost-Benefit Analysis model using the optional overhead line, it is worth pointing out as a cost category. One common example of this is overtime pay needed to cover for unexpected leave by an abstractor. Smartsourcing has NO unknown costs. Clients pay by the chart, so budgeting is clear and straightforward.
Opportunity Costs
An opportunity cost refers to the value of what you lose when you chose between two or more options. Every decision has trade-offs, and opportunity cost signifies the potential benefits you’ll miss out on by choosing one direction over another.
Department Leadership Time & Focus
 One of the most commonly overlooked opportunity costs of an in-house team is the department leadership’s time and focus. Any amount of time spent staffing and managing data abstraction is time not spent on bigger picture strategic work like scrutinizing your quality data to identify areas of improvement, designing initiatives to drive change, and monitoring and measuring success.
One of the most commonly overlooked opportunity costs of an in-house team is the department leadership’s time and focus. Any amount of time spent staffing and managing data abstraction is time not spent on bigger picture strategic work like scrutinizing your quality data to identify areas of improvement, designing initiatives to drive change, and monitoring and measuring success.
To attempt to quantify the opportunity cost of the time spent staffing and managing an abstraction staff, consider the findings from a large study of 32,410 people by research firm Leadership IQ and featured in Fast Company. The study found that the most effective and motivated employee gets 6 hours per week from their manager, including email communication, group meetings, 1-on-1 meetings, and cumulative face-to-face or phone conversations.
As group meetings and email communication overlap with multiple employees at once, a manager of 5 abstractors likely shouldn’t estimate 6 full hours per week for each employee, which would amount to 30 hours of doing nothing but managing those 5 team members. But 6 hours or 15% of a manager’s 40-hour work week is the minimum amount of time that should be incorporated into a Cost-Benefit Analysis. Using our example, the average salary for a hospital department manager is $109,840 in Georgia. Assuming only 15% of their time is spent managing abstraction staff, that’s an opportunity cost per year of $16,476 or 312 hours (nearly 8 full work weeks). ADN’s Cost-Benefit Analysis Template allows you to adjust this percentage upward from 15% if your team is larger than 1 or 2 abstractors.
Turnover Costs
Turnover is a substantial drain on both management and fellow abstractors when one considers all the time that goes into recruiting, hiring, and especially training. In 2022, the hospital turnover rate for RNs climbed dramatically to 27.1%, up from 18.7% in 2021, meaning the average expected tenure is now 4 years down from 5, according to the 2022 NSI National Health Care Retention & RN Staffing Report. A survey conducted as part of that report found that the average cost of turnover of an RN is $46,100. So given that a turnover event on average will occur every 4 years, that total turnover cost translates into $11,525 per year of indirect costs.
Strategic ROI & The 4 Stages of Data Maturity
Strategic ROI #1: More Strategic Use of Clinical Personnel as Active Change Agents Instead of Passive Data Collectors
Healthcare organizations on the leading edge of quality improvement are reinventing their approach to data, focusing less on adding ever more data to an information black hole and instead organizing more resources around producing insight from the data and, most importantly, acting on the data to effect change for the better. This doesn’t mean they neglect data collection. Rather, they’re smarter in how they collect it by leveraging AI and outsourcing partners to handle the more routine aspects of data collection so they can focus their precious and scarce personnel resources on more advanced roles like analysts and change agents.
The 4 Stages of Data Maturity
Over the years, many organizations to varying degrees of success have embarked on journeys to become “High Reliability Organizations.” But all healthcare organizations, whether they realize it or not, are on a Journey to Data Maturity. Some facilities are more clear-eyed than others about this concept while some may not realize they have stalled on this journey. So ADN developed a tool, the “Hierarchy of Data Maturity”, to help organizations honestly assess their approach to data and benchmark their current actual performance against the goal of reaching the promised land of data maturity.
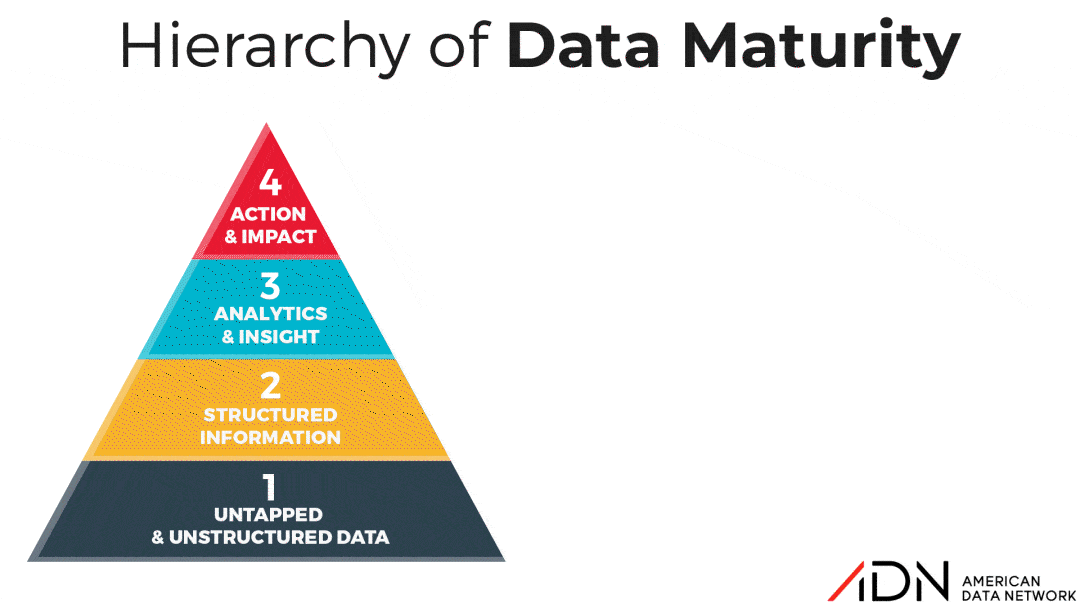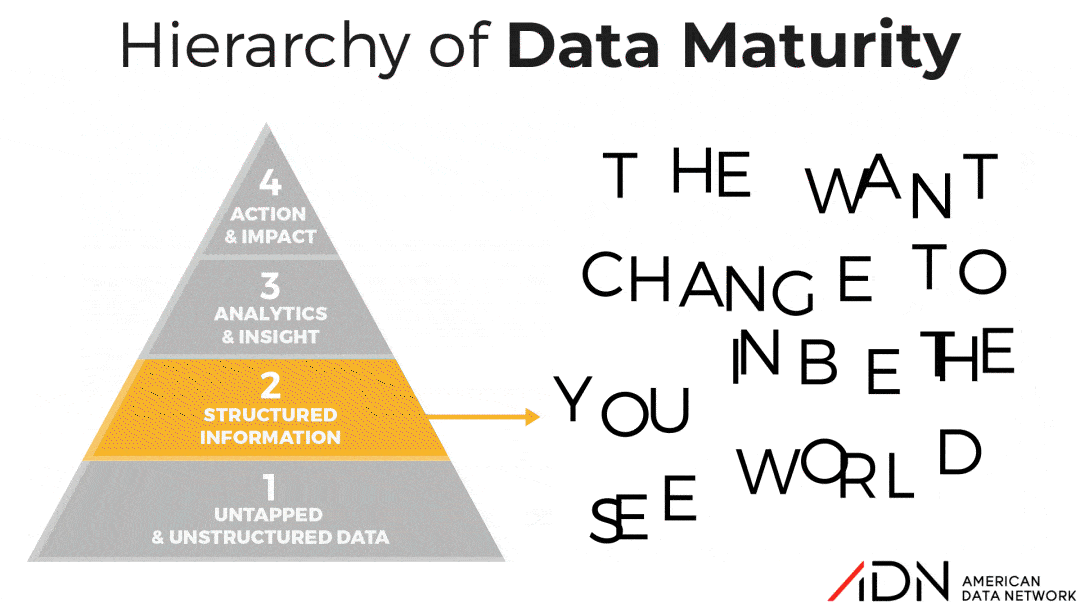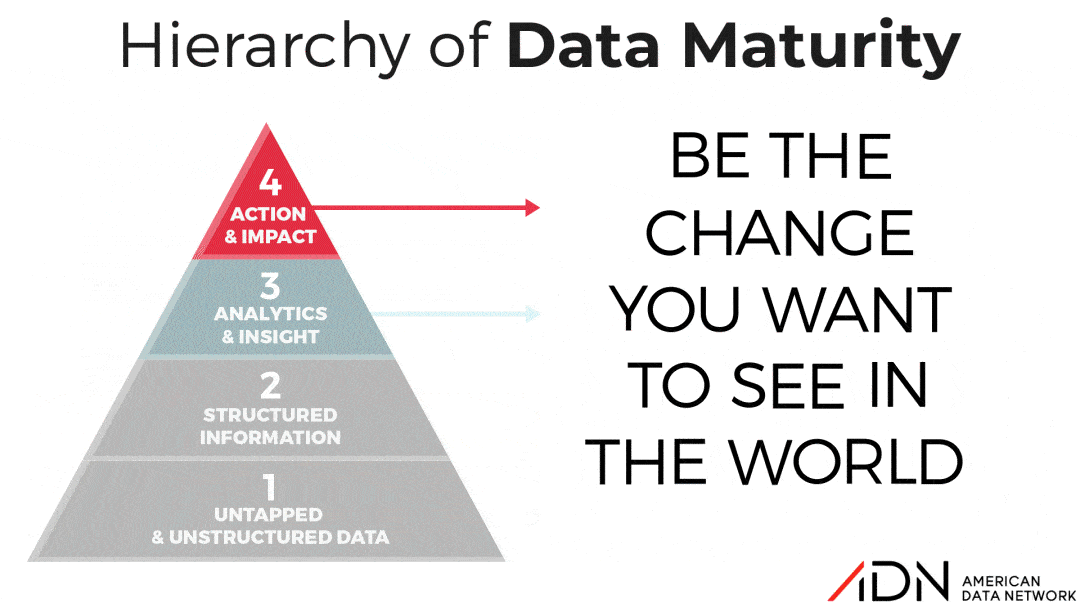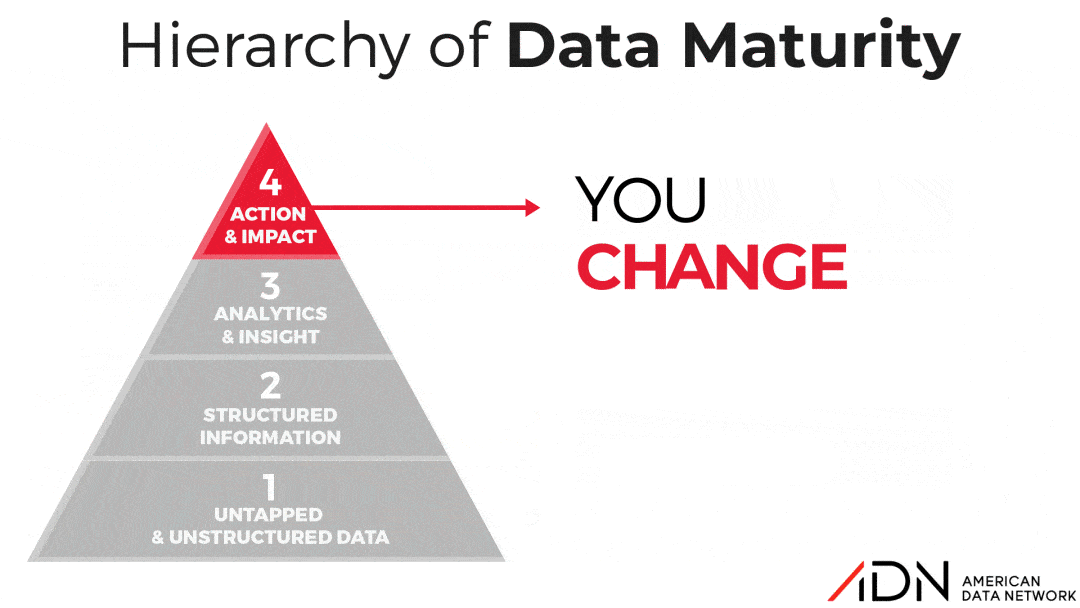
Stage 1: Untapped & Unstructured Data
In this stage, data about key performance indicators is generated but not actively collected or organized in a way that can be analyzed, resulting in irregularities and ambiguities. Fortunately, most healthcare organizations have progressed out of this stage thanks to the proliferation of EHRs, other electronic data reporting tools like patient safety event reporting applications, and the development of common format data frameworks like Core Measures and other registries for surgery, stroke and cardiovascular treatment, etc.
Stage 2: Structured Information
Unfortunately, many organizations have stalled in this stage. They spend a lot of time and have marshaled a lot of personnel resources around collecting and organizing data, but not nearly as much time and resources analyzing and acting on the insight produced by the data. Much of this grew out of the “meet the mandate” mentality. Organizations mobilized resources to meet data collection mandates by the Center for Medicare and Medicaid Services and The Joint Commission. But then competing priorities, skill gaps, or any number of other reasons caused these organizations to stall rather than progress upward in data maturity.
Stage 3: Analytics & Insight
Organizations in this stage conduct regular and frequent analyses of their quality and safety data. And while these facilities are better at identifying opportunities for improvement than those in the stage below, action is often hampered by competing priorities. This usually indicates that the personnel charged with acting on the quality and safety data have multiple, if not too many, job functions. This tends to lead to an operational bottleneck that shrinks the number of performance improvement initiatives that might otherwise occur if the teams were better organized around data action in the ways organizations at the pinnacle of data maturity are.
Stage 4: Action & Impact
This is the promised land, where all of an organization’s data efforts come to a point, literally, to effect change for the better. Organizations in this stage often have entire analytics or informatics teams or even departments whose primary goal is to mine clinical data for opportunities for improvement, then operationalize initiatives that fine-tune care quality and safety. Many quality departments doing this well have assembled teams that include both individuals with a background in informatics as well as internal rising stars who were former data abstractors and already have a deep understanding of internal processes and gaps, thus can more easily identify root causes and corrective actions.
Perhaps the greatest value of smartsourcing data abstraction is that it helps an organization make better strategic use of personnel for performance improvement. Data is one of the most important assets that health systems have, yet most do not have the time, resources, or plan in place to maximize the value. To move the needle and thrive, leaders must direct more staff time to data management and improvement efforts. Having a trusted outsourcing partner who can handle the routine data collection empowers an organization to refocus scarce clinical team members on more impactful functions like being active change agents rather than passive data collectors.
And that type of strategic shift is the sort of change that propels an organization further up the data maturity pyramid. Loma Linda University Health, in this case study, details multiple process improvement projects and associated ROI that resulted from their repurposing of former abstractors to more active PI roles. This leading California health system’s VP of Quality and Safety shares how several of the initiatives they conducted were made possible by having their former abstractors focus primarily on process improvement. The initiatives they spearheaded resulted in better compliance and led to more consistent reimbursements. In fact, their Epic PI Project around Proactive Visibility into Stroke Treatment was so compelling, they were chosen to speak at the National Epic Conference.
Strategic ROI #2: Improved Leadership Focus
Clinging to departmental functions like routine data collection carries a major opportunity cost — the department leader’s time and focus. Any amount of time spent staffing and managing data abstraction is time not spent on bigger picture strategic work like scrutinizing quality data to identify areas of improvement, designing initiatives to drive change, and monitoring and measuring success.
Strategic ROI #3: Solve Turnover (For Good)
Average turnover for hospitals climbed from 18.7% in 2021 to an excruciating 25.9% in 2022, according to the 2022 NSI National Health Care Retention & RN Staffing Report. Moreover, the cost burden related to turnover of a nurse (recruiting/hiring/training) is $46,100. And the difficulty index of hiring a skilled nurse is 3 months (87 days), perhaps longer for the specialized position of a data abstractor.
Furthermore, turnover is a substantial time-drain and diversion of focus for the department manager and forces the remaining abstraction team to shoulder the workload burden, often unsuccessfully resulting in a substantial backlog. In many instances when turnover happens, the department manager or Quality Director even has to roll up his or her sleeves to step in and assist with abstractions, as was the case detailed in this case study.
Partnering with a trusted data abstraction outsourcing company like ADN completely eliminates the problem of abstractor turnover for the hospital, as we have a much larger team of abstraction experts than a hospital would have, with redundancies built-in for when we have turnover.
Strategic ROI #4: Seamless Performance Despite Temporary or Extended Leave (Illness, Maternity Leave, PTO)
Some organizations are learning the hard way that not having a backup plan in place for an abstractor’s temporary or extended leave like PTO, illness, or maternity leave can cause major disruptions. In such an event, a backlog can pile up as other abstactors, even with overtime, may not be able to handle the additional workload. Often, individuals far too senior like the Quality Director can get pulled into abstracting to try to prevent a backlog or data gap, which, needless to say, is not a prudent use of their skills and experience. On the flip side, short staffing can also cause individuals far too inexperienced to get tapped to help, which is unlikely to produce reliable data that you want driving your priorities and practice patterns.
Many clients use ADN in addition to their in-house abstraction team so that in the event of temporary or extended leave, we can seamlessly handle the additional caseload while the team member is out given the depth and breadth of our team of abstraction experts.
Strategic ROI #5: Enhanced Employee Engagement
Another benefit of outsourcing is the positive emotional and career impact it can have for rising-star abstractors ready for more growth and responsibility. And given the skyrocketing burnout rate, there’s never been a more opportune time for leaders to prioritize the engagement and fulfillment of their high-performing team members.
Many organizations elevate those individuals to roles primarily focused on using the data they once abstracted for performance improvement initiatives, as detailed in this case study of Loma Linda University Health.
“All of my individuals who did abstraction previously are nurses. So for them to see that their knowledge of the data, workflows, and processes and their contribution with the team in making care better for patients, that’s invaluable,” said Loma Linda’s Assistant Vice President of Quality & Patient Safety. “Because they then get to look at what’s happened with our data outcomes, celebrate those things, and move on to the next area of opportunity. It’s very fulfilling to those individuals. It is important to folks to know that the work that they’re doing is positively impacting patient outcomes.”
Key Takeaways
Quality teams are not passive collectors of data anymore. While this may have been true 10 years ago, the authority and significance of the quality department has elevated beyond that and is continuing to command even more importance at the leadership table in healthcare. Holding on to the management of routine data collection is taking up too much of your valuable time. Any amount of time spent staffing and managing data abstraction is time not spent on bigger picture strategic work like scrutinizing your quality data to identify areas of improvement, designing initiatives to drive change, and monitoring and measuring success. Instead, focus that time you free up on using the data we abstract for bigger, more impactful work that can help you elevate your professional impact on moving your department and organization forward.
FREE TOOLS
- Data Abstraction Outsourcing Cost Benefit Analysis Calculator
- ADN’s Abstraction Team Resume – If you’re still considering filling roles that become vacant through natural attrition, compare our team’s resume to potential hires.
- Strategic and Tactical Benefits of Smartsourcing


 One of the most commonly overlooked opportunity costs of an in-house team is the department leadership’s time and focus. Any amount of time spent staffing and managing data abstraction is time not spent on bigger picture strategic work like scrutinizing your quality data to identify areas of improvement, designing initiatives to drive change, and monitoring and measuring success.
One of the most commonly overlooked opportunity costs of an in-house team is the department leadership’s time and focus. Any amount of time spent staffing and managing data abstraction is time not spent on bigger picture strategic work like scrutinizing your quality data to identify areas of improvement, designing initiatives to drive change, and monitoring and measuring success.


